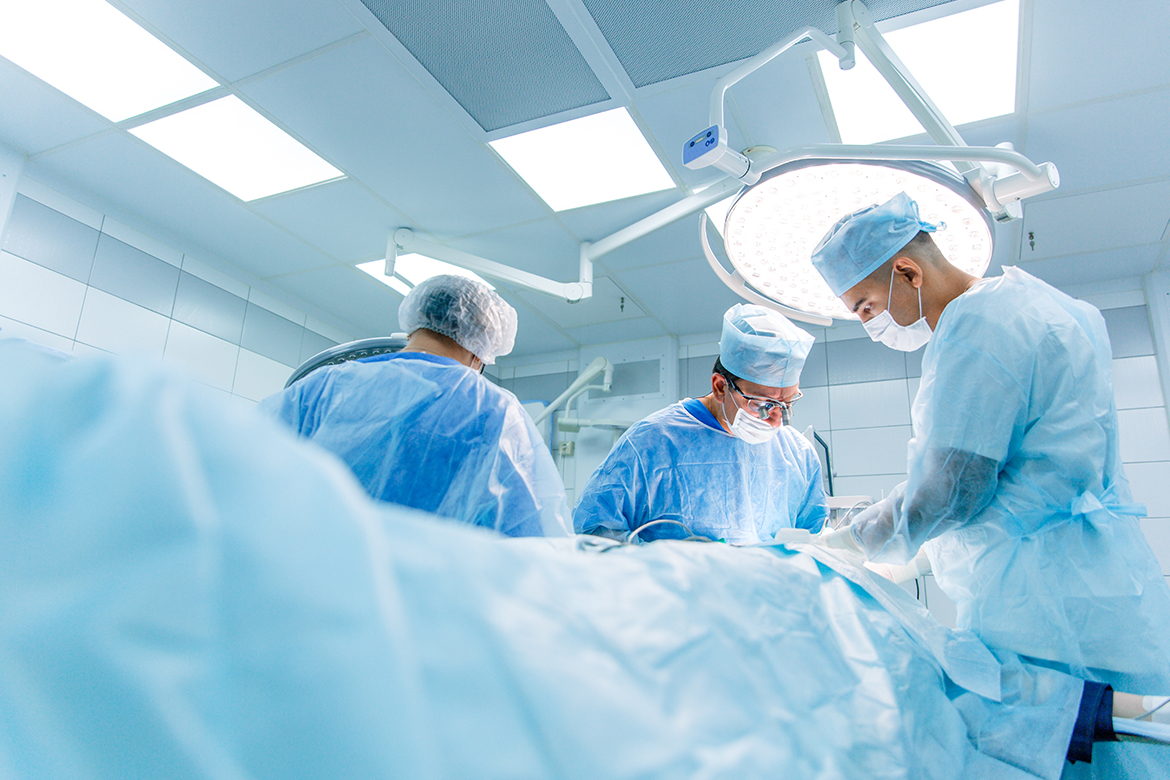
“Anaesthesia” for awake craniotomy is a unique clinical setting that needs the anaesthesiologist to provide variable states of sedation and analgesia, to ensure optimal patient comfort without compromising the electrophysiological monitoring and patient cooperation, but also to manipulate cerebral and systemic haemodynamics while ensuring adequate ventilation and airway safety. Awake craniotomy is the main surgical option for intraoperative mapping and subsequent resection of lesions located in the close proximity of the eloquent brain tissue in order to minimize brain damage. It is a challenging situation for the surgical and the anesthesia teams as there is little room for error in an awake patient whose participation and cooperation is integral to overall success of the surgery. The patient is briefed about all the steps of the planned procedure including need for prolonged immobilization as this procedure would be a life-changing or a life-altering experience for the patient. Efforts should be taken by all the treating teams to minimize anxiety and stress of the patient. A successful surgery begins with meticulous planning using all the available technological innovations to identify the lesion and its relation with important functionally eloquent areas of the brain. Intraoperative monitoring of neurological functions is a crucial aspect of the surgery and patients should be fully alert, cooperative and responsive to the testing. Neurological functions that are tested include gross motor, fine motor and speech functions. Speech testing includes language fluency, repetition, recall, object naming and calculations. A preoperative baseline assessment of neurological functions and counselling of patient for intraoperative testing is necessary to gain patient’s faith and trust in the monitoring team. A good rapport is thus created between the patient and the monitoring team which is useful during intraoperative monitoring.

Keeping the patient awake, alert and cooperative during intraoperative testing while simultaneously providing a pleasent, painless experience is the role of the anaesthesiologist. Planning an ideal anaesthetic regimen tailored to a particular patient and neurological function to be monitored is absolutely essential. The patient can either be kept awake throughout the surgery or only during the testing phase and asleep during other parts of the surgery. The level of sedation should be titrated to avoid over-sedation and its related undesirable effects.
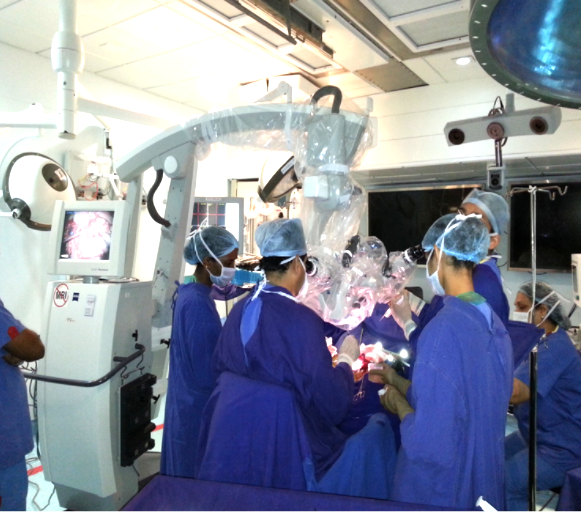
Teamwork, meticulous planning with proper selection of the patient along with use of technological advances and vigilant intraoperative monitoring of neurological functions help in making this challenging surgery a pleasant and rewarding surgery.
 Back to Site
Back to Site