Brain tumours are the commonest cancers seen in children after blood cancers like Bleukaemias and lymphomas. However, they are rarely recognised or diagnosed at an early stage. This article discusses the warning signs and symptoms that should alert a practitioner about the possibility of a brain tumour in a child.
Predisposing Factors
Statistically, brain tumours are more likely in those children with a family history of cancer. Other predisposing factors include a history of previous cranial radiotherapy, or in those suffering from tuberous sclerosis, neurofibromatosis and other familial genetic syndromes.
Symptoms
- Headaches
- Vomiting
- Visual difficulties
- Neurological weakness
- Change in behaviour or educational abilities
- Seizures
- Increase in the head circumference
- Polyuria/polydipsia
Signs
- Cranial nerve abnormalities
- Cerebellar signs
- Papilloedema
- Reduced level of consciousness
- Other neurological signs
Brain Tumours have the longest delay between the appearance of symptoms & diagnosis
When Should We Think Of A Brain Tumour?
Growth of brain tumours depend upon their biological nature. With slow growing tumours, non specific signs and symptoms, such as headache or vomiting may be present for quite some time before a CNS cause is suspected. Symptoms and signs are usually due to pressure on the surrounding structures or due to raised intracranial tension.
Headaches: Any new persistent headache that lasts for more than four weeks must be investigated. This is especially true for early morning headaches. For younger children confusion, disorientation or a change in behaviour may be the clue to the diagnosis.
Pitfall: Not reassessing a child with a migraine or a tension headache when the character of the headache changes.
Nausea & Vomiting: Any persistent nausea and vomiting that lasts for more than two weeks or any early morning vomiting must be investigated with an MRI scan.
Pitfall: Not thinking of a CNS cause in cases of nausea and vomiting.
Change in Vision: Consider a brain tumour in any child with a visual problem that lasts for more than two weeks. Assessment should include acuity and field of vision, eye movements, pupil responses and fundoscopy.
Pitfall: Not recommending imaging in conditions like papilloedema, optic atropy, proptosis, new onset nystagmus/squint and non-refractive reduction in visual acuity.
Motor Dysfunction: CNS imaging should be obtained in any child with abnormalities in gait/co-ordination, focal motor weakness or swallowing difficulties without a local cause. Sometimes, changes can be quite subtle, such as a sudden change in hand preference in a child.
Pitfall: Not identifying swallowing difficulties that could be due to underlying neurological problem or attributing abnormalities in gait/balance to middle ear disease.
Growth & Development: A brain tumour should be considered in any child presenting with a regression in motor skills, inappropriate increase in head circumference or in any combination of growth failure, delayed puberty and polyuria/polydipsia.
Pitfall: Not considering a CNS cause in a child presenting with vomiting and weight loss, and failing to consider diabetes insipidus in a child with polyuria/polydipsia.
Behavioural Changes: Lethargy is the commonest behavioural abnormality that occurs with brain tumours.
Pitfall: Not suggesting further investigations in a child who is lethargic in situations wherein he/she is normally active.
Investigations
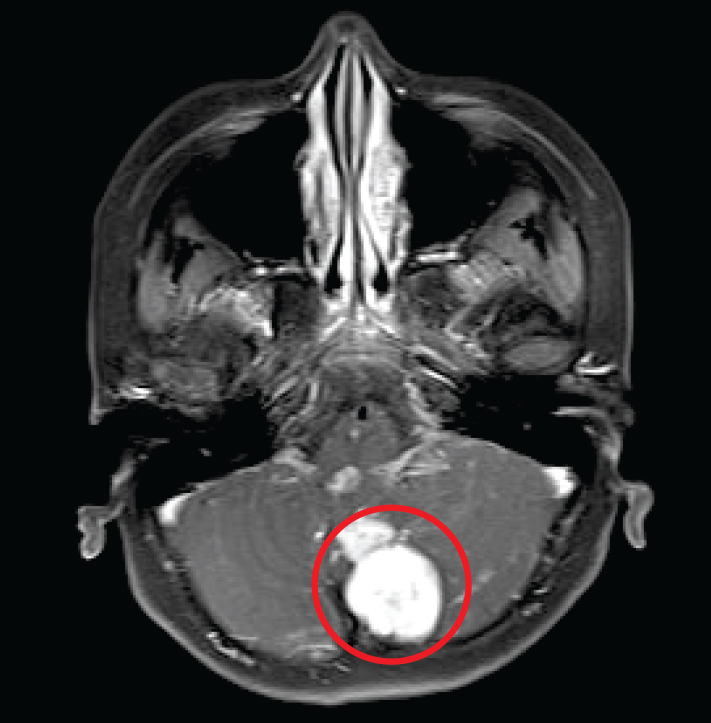
Brain tumours have the longest delay between the appearance of symptoms and diagnosis. The mean delay between symptoms and diagnosis is nearly three months, which means that outcome is also adversely influenced. In suspected cases of brain tumour, an MRI with contrast enhancement is the modality of choice. This is because a CT scan may not pick up minute abnormalities that are apparent on an MRI scan
Overcoming The Common Pitfalls
The initial symptoms of a brain tumour frequently mimic those that occur with other common childhood illnesses. Symptoms may fluctuate, disappear and recur over time, and this does not exclude a brain tumour and neither does an initial normal neurological examination. One needs to be vigilant about unusual and/or persistent symptoms, and if worried, a proper imaging with an MRI scan should always be obtained.
 Back to Site
Back to Site