Trauma is the leading killer, especially in children. In children, mortality due to Traumatic Brain Injury (TBI) is high (~ 60%) because of a large head to body surface ratio, higher water content and less myelination.
The mechanisms of injury can be direct injury to the brain like contusional (coup & contre coup) or shear injury (white matter tracts, diffuse axonal injury) and extra-axial collections (epidural, subdural, subarachnoid and intraparenchymal). Neuronal death following head injury may occur early, primary (Non-Preventable) or late due to secondary (Preventable) injury. Secondary neuronal injury can be prevented by avoiding insults which would compromise cerebral blood flow and oxygenation. Sustained, pathological rise in Intracranial Pressure (ICP) compromises the cerebral blood flow, thereby aggravating the brain injury (Munroe-Kellie Principle). Management of intracranial hypertension is the cornerstone in the management of traumatic brain injury.
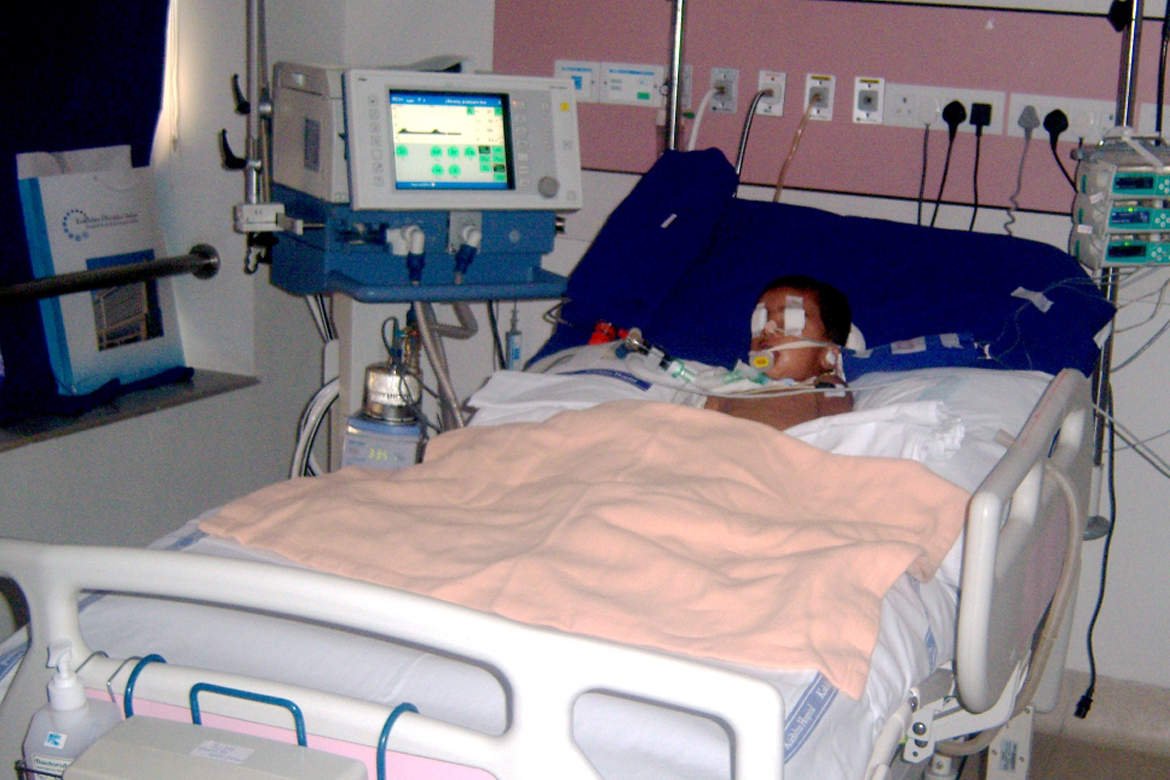
Principles of Management of TBI include
- Aggressive Control of ICP
- Maintain Optimum MAP (CPP)
- Avoid Hypoxia/Hypercarbia
- Avoid Hyperthermia
- Avoid Hyponatremia
- Maintain Normoglycemia
- Minimise Cerebral Metabolism
CT brain is the neuroimaging of choice in TBI. Precautions for suspected C-spine injury are essential until cervical spine is clinically cleared.
ICP Guided Therapy, by continuous monitoring of intracranial pressure by using External Ventricular Drain (EVD) or intraparenchymal probes (e.g.: Codman’s catheter) has shown better outcomes. Aggressive control of ICP and good nursing care forms the mainstay in the management of TBI. TBI management guidelines should be in place in all the nursing homes to prevent secondary brain injury which will improve both the morbidity and mortality in these children.
| Severity of Traumatic Brain Injury (TBI) by Glasgow Coma Scale (GCS) | |
| Mild | GCS score of 13 or higher, possibly symptoms of disorientation, altered mental status or vomiting |
| Moderate | GCS score of 9 to 12 |
| Severe | GCS < 9 |
Trauma is the leading killer, especially in children.
Management in ER
- Endotracheal Intubation – RSI
- Controlled Ventilation- PaCO2 ~35 mm Hg
- Oxygen Saturation >95%
- Fluid Resuscitation – Adequate MAP
- Adequate Haemostasis
- Sedation and Paralysis
- Seizure Control
Stat CT scan of the head and neurosurgical consult if uncontrolled intracranial hypertension or signs of herniation develop.
Management of Raised ICP in ICU
- Elevate Head of Bed (30 degrees)
- Keep Head Mid-Line, C-Spine Precautions
- Ventilation to PaCO2 35 mmHg
- Maintenance of Normal Temperature
- Isotonic Fluids at Maintenance Levels
- Muscle Paralysis and Sedation
- Seizure Control
- Aggressive Control of Raised ICP – Hyperosmolar Therapy (3% NaCl, Mannitol), Hyperventilation, Therapeutic Hypothermia, Barbiturate Coma & Decompressive Craniotomy)
- Optimum Nutrition
 Back to Site
Back to Site